Introduction
Welcome to The Diageo Healthcare Scheme guide.
Diageo have appointed us, Healix Health Services Ltd, to manage this scheme. Our role is to assess and manage medical needs that you might have as well as the care and treatment you receive.
The Diageo Healthcare Scheme is designed to cover you for the diagnosis and/or treatment of a short term medical condition, if the treatment is medically necessary.
The scheme is not intended to cover all medical conditions. There are some medical conditions and treatments that are excluded from cover (please see exclusions and limitations for further details on this).
All treatment (including consultations and diagnostic tests) should be authorised in advance. Therefore it is essential that you call us before you receive treatment, to ensure that your proposed treatment is eligible for cover under the scheme.
If you would like your partner or dependants to be covered under the healthcare scheme, regardless of their gender, please contact your HR department who will advise you if this is possible.
Table of benefits
Your scheme benefits are outlined in the table below.
Please note, the below benefits are:
-
subject to an excess
Benefit limits apply per member, per scheme year unless otherwise stated. Once a benefit limit is reached, no further cover will be provided within the scheme year specified below. Cover for continued consultations, diagnostics or treatment in the next scheme year will be subject to all healthcare scheme terms and conditions.
The scheme year will commence on the 1st January 2026 - 31st December 2026
| Benefit Type | Level of Cover | Benefit Note |
| Outpatient Diagnostics and Treatment | ||
Outpatient diagnostics and consultations with a specialist or practitioner following GP or specialist referral (self-referral available for specified cancer symptoms) |
Full cover | 1a |
Outpatient treatment and surgical procedures |
Full cover | 1b |
Outpatient MRI, CT and PET scans following specialist referral |
Full cover | 1c |
Monitoring of a chronic condition |
Up to £1,000 per scheme year | 1d |
Neurodevelopmental disorder assessment |
Up to £2,000 per scheme lifetime | 1e |
Orthotics |
Up to £500 per scheme lifetime | 1f |
| Inpatient and Day Case Treatment | ||
Specialist fees and hospital charges for inpatient and day case treatment |
Full cover | 2a |
Parent accommodation - hospital |
Full cover | 2b |
| Therapies | ||
In-network outpatient physiotherapy (including self-referral) |
Full cover | 3a |
Out-of-network outpatient physiotherapy following GP referral |
Up to £350 per scheme year | 3b |
Out-of-network outpatient physiotherapy following specialist referral |
Full cover | 3c |
Outpatient complementary therapies following GP or self-referral |
Up to £350 per scheme year | 3d |
Outpatient complementary therapies following specialist referral |
Full cover | 3e |
| Mental Health | ||
In-network outpatient mental health treatment (including self-referral) |
Full cover | 4a |
Out-of-network outpatient mental health treatment |
Up to £1,500 per scheme year | 4b |
Inpatient and day case mental health treatment |
Up to 28 days per scheme year | 4c |
| Cancer Treatment | ||
Cancer treatment |
Full cover | 5a |
Wigs |
Up to £125 per scheme lifetime | 5b |
Mastectomy bras |
Up to £125 per scheme lifetime | 5c |
| Cash Benefits | ||
NHS cash benefit |
£200 each day or night | 6a |
NHS cash alternative |
Up to 25% of the costs to receive the procedure privately | 6b |
NHS cancer cash benefit |
£300 each day or night | 6c |
NHS cancer cash benefit for oral chemotherapy and targeted therapies |
£600 per month | 6d |
Baby cash benefit |
£100 per child | 6e |
NHS cancer screen cash benefit |
Up to £25 per screen | 6f |
| Additional Benefits | ||
Fertility investigations |
Full cover | 7 |
Fertility treatment |
Up to £10,000 per scheme lifetime | 8 |
Gender dysphoria |
Up to £10,000 per scheme lifetime | 9 |
Biofeedback |
One course of treatment per scheme lifetime | 10 |
Women's and Men's Health benefit Remote advice service with our in-network experts (up to 4 consultations per scheme year) Diagnostics following referral from our in-network experts (up to £500 per scheme year) |
Limited cover | 11 |
Private ambulance charges |
Full cover | 12 |
Home healthcare |
Full cover | 13 |
Overseas emergency treatment |
Limited cover | 14 |
Please note: the above benefits only apply when consultations, diagnostics or treatment take place in the UK unless specified otherwise.
Outpatient Diagnostics and Treatment
We will pay in full for:
- outpatient consultations with a specialist or practitioner following GP referral
- outpatient consultations with a practitioner following specialist referral. The practitioner must be registered with the correct governing body for their field, and meet our definition for a practitioner
- outpatient diagnostics following specialist referral
Please note: cover is subject to our reasonable and customary fees. See exclusions and limitations for details of treatment that is not eligible for benefit.
Outpatient Consultations with a Specialist on Self-Referral for Specified Cancer Symptoms
We will pay in full for self-referred consultations and diagnostics for specified cancer symptoms.
Refer to the self-referred cancer benefits section for further information on symptoms that are eligible, and how to access this benefit.
If a diagnosis of cancer is made, cover for eligible treatment will be subject to any limits as outlined in your cancer treatment benefit.
Back to topWe will pay in full for hospital charges and specialist fees for outpatient treatment, surgical procedures and drugs and dressings used during an outpatient appointment.
Cover is subject to our reasonable and customary fees.
Back to topWe will pay in full for MRI, CT and PET scans following specialist referral.
Back to topWe will pay up to £1,000 per scheme year for the below when required to monitor a chronic condition:
- outpatient consultations with a specialist following GP referral
- outpatient diagnostics following GP or specialist referral
Once this benefit limit has been reached the chronic condition rule applies, as outlined in your exclusions and limitations.
Please note, this benefit includes mental health treatment for mental health conditions.
Back to topWe will pay up to £2,000 per scheme lifetime for the assessment of neurodevelopmental disorders, following GP or specialist referral. The assessment must be carried out by a specialist or educational psychologist that we recognise for benefit purposes.
You must have our confirmation before any assessment is carried out, and we will need full clinical details from your GP or specialist before we can confirm cover.
Once a diagnosis has been confirmed, there will be no further cover for any additional assessments, consultations, diagnostics or neurodevelopmental disorder treatments.
Back to topWe will pay up to £500 per scheme lifetime towards medically necessary orthotics, when these are recommended by a GP, practitioner, physiotherapist or specialist.
Back to topSpecialist Fees
We will pay specialist fees in full for inpatient and day case treatment. Cover is subject to our reasonable and customary fees.
Hospital Charges
We will pay hospital charges in full for the following:
- accommodation and nursing care for inpatient or day case treatment
- operating theatre and recovery room
- prescribed medicines and dressings, for use whilst an inpatient or for day case treatment
- eligible surgical appliances - for example, a knee brace following ligament surgery
- prosthesis or device which is inserted during eligible surgery
- pathology, radiology, diagnostics, MRI, CT and PET scans
- physiotherapy received during inpatient or day case treatment
- intensive care
- short-term dialysis when needed temporarily for sudden kidney failure resulting from an eligible condition or treatment
- skin and corneal grafts
We will pay reasonable hospital costs for one parent or legal guardian to stay with a child who is under 16 years old, if a child is admitted to hospital as an inpatient.
Cover for this benefit will stop on the child’s 16th birthday. If your child is an inpatient on their 16th birthday, then cover will extend until they are discharged on that occasion.
We will only pay the cost if:
- it is the parent or legal guardian who stays with the child, and
- the treatment the child receives is covered by the scheme
We will pay in full for outpatient physiotherapy following GP, specialist or self-referral when provided by our physiotherapy network provider.
You also have access to a digital triage service via the Member Zone / the My Healix App. This service is not subject to your excess, your scheme underwriting or any benefit limits (if applicable) when accessed through our digital pathway provider.
Refer to the musculoskeletal pathway section for further information.
Back to topWe will pay up to £350 per scheme year for outpatient physiotherapy following GP referral, when taken outside of our physiotherapy network. The physiotherapist must be recognised by us for benefit purposes.
Cover is subject to our reasonable and customary fees.
Please note, you also have access to a digital triage service via the Member Zone / the My Healix App. This service is not subject to your excess, your scheme underwriting, or any benefit limits (if applicable) when accessed through our digital pathway provider. Refer to the musculoskeletal pathway section for further information.
Back to top
We will pay in full for for outpatient physiotherapy following specialist referral, when taken outside of our physiotherapy network. The physiotherapist must be recognised by us for benefit purposes.
Cover is subject to our reasonable and customary fees.
Please note, you also have access to a digital triage service via the Member Zone / the My Healix App. This service is not subject to your excess, your scheme underwriting, or any benefit limits (if applicable) when accessed through our digital pathway provider. Refer to the musculoskeletal pathway section for further information.
Back to topWe will pay up to £350 per scheme year for chiropractic treatment, osteopathy and acupuncture following GP or self-referral. You must be referred to a complementary practitioner we have recognised for benefit purposes.
Back to topWe will pay in full for chiropractic, osteopathy and acupuncture sessions, following specialist referral. The complementary practitioner recognised by us for benefit purposes.
Cover is subject to our reasonable and customary fees.
Back to topWe will pay in full for outpatient consultations and mental health treatment for eligible mental health conditions following GP, specialist or self-referral, when provided by our mental health network provider.
Please note, you also have access to a digital triage service via the Member Zone / the My Healix App. This service is not subject to your excess, your scheme underwriting, or any benefit limits (if applicable) when accessed through our digital pathway provider.
Refer to the mental health pathway section for further information.
Please note, under 18s will require a referral letter from a GP or specialist.
Where treatment is for an addiction treatment programme, cover is limited to once per scheme lifetime. Treatment must be recommended by a GP or specialist and carried out by one of our network providers as an inpatient or remotely. Treatment will be subject to the 28-day limit detailed in this benefit.
Back to topWe will pay up to £1,500 for outpatient consultations and mental health treatment for eligible mental health conditions following GP or specialist referral, when taken outside of our mental health network. The psychological therapist must be recognised by us for benefit purposes.
Cover is subject to our reasonable and customary fees.
Please note, you also have access to a digital triage service via the Member Zone / the My Healix App. This service is not subject to your excess, your scheme underwriting, or any benefit limits (if applicable) when accessed through our digital pathway provider. Refer to the mental health pathway section for further information.
Back to topWe will pay up to 28 days per scheme year for eligible inpatient and day case mental health treatment.
You must be under the direct care and supervision of a consultant psychiatrist, and receive authorisation from us in advance and in writing.
Where treatment is for an addiction treatment programme, cover is limited to once per scheme lifetime. Treatment must be recommended by a GP or specialist and carried out by one of our network providers as an inpatient or remotely. Treatment will be subject to the 28-day limit detailed in this benefit.
Back to topWe will pay for cancer treatment as outlined in the cancer cover explained section.
For information on additional services available, refer to the cancer support explained section.
Back to topWe will pay up to £125 per scheme lifetime towards the cost of a wig if you need one due to hair loss caused by cancer treatment
This benefit is available on a pay and claim basis only.
Back to topWe will reimburse up to £125 per scheme lifetime for the cost of mastectomy bras required following eligible cancer treatment.
This benefit is available on a pay and claim basis only.
Back to topIn the event that you are admitted to an NHS hospital, or you elect to receive treatment through the NHS that incurs no cost to the scheme, we will pay a cash benefit of £200 per day for day case treatment or £200 per night following inpatient treatment.
This benefit cannot be claimed alongside any other benefit and will only apply to claims for inpatient or day case treatment that would otherwise have been eligible for benefit under the scheme. NHS emergency admissions are not eligible for NHS cash benefit for the period of time spent in an emergency department or assessment unit.
For details on how to claim this benefit please click here.
Back to top
In the event that you require an elective surgical procedure, and you choose to receive this treatment free of charge on the NHS, we may pay you a cash lump sum. Please contact us to check if your procedure will qualify for this benefit.
For details on how to claim this benefit please click here.
Back to topIn the event that you elect to receive free cancer treatment through the NHS, we will pay an NHS cancer cash benefit of £300 per day for day case treatment, or £300 per night for inpatient treatment, or £300 per outpatient radiotherapy treatment appointment.
This benefit will only apply to claims for inpatient or day case treatment that would otherwise have been eligible for benefit under the scheme.
For details on how to claim this benefit please click here.
Back to topIn the event that you elect to receive oral chemotherapy or targeted therapies via the NHS as an outpatient, we will pay a cancer cash benefit of £600 per month.
For details on how to claim this benefit please click here.
Back to topWe will pay a cash benefit of £100 per baby / child following birth or adoption, where either one or both parents are members of the scheme. This benefit can only be claimed once per baby / child, even if both parents are covered under the scheme.
For details on how to claim this benefit please click here.
Back to topIn the event that you are invited to attend an NHS cancer screening service for bowel, breast or cervical cancer free of charge on the NHS we will pay an NHS cancer screen cash benefit of £25 per screen following your attendance.
Back to topWe will pay in full for medically necessary fertility investigations following GP or specialist referral.
Once a diagnosis has been confirmed, there will be no further cover for any additional consultations, diagnostics or fertility treatment in the future.
Back to topWe will pay up to £10,000 per scheme lifetime for fertility treatment as outlined in the fertility treatment explained section.
Back to topWe will pay up to £10,000 per scheme lifetime for gender dysphoria as detailed in the gender dysphoria explained page.
Back to topWe will pay in full for one course of biofeedback, a maximum of 5 sessions, per scheme lifetime. This will cover treatment for irritable bowel syndrome and gastrointestinal symptoms, including constipation and faecal incontinence on specialist referral. We will require full clinical details from your specialist before we can give our decision on cover. Treatment must be carried out by a registered nurse or physiotherapist.
Back to topRemote Advice Service with Our In-Network Experts
We will pay for up to 4 remote advice appointments per scheme year with our in-network experts, following self-referral. This service can be used to discuss any health concern including conditions that are normally excluded from cover such as the menopause, andropause, sexual health concerns, fertility or contraception advice.
Diagnostics Following In-Network Expert Referral
We will pay up to £500 per scheme year for diagnostics that are recommended following a remote advice appointment with our in-network experts.
Refer to the women’s or men’s health services section for further information on how to access these benefits.
Once either benefit limit has been reached, the scheme rules will apply as outlined in your exclusions and limitations.
Please note: The above benefits will not be subject to an excess, where this applies. Additional cover may be available outside of the above limits for eligible claims, please contact us for further information.
Back to topWe will pay in full for transport by a private ambulance to and / or from a hospital when ordered for medical reasons.
Back to topWe will pay in full for home nursing charges with a registered nurse when recommended by a specialist and where it is:
-
medically necessary and without it you would have to receive treatment as an inpatient or day case admission, and
-
needed for medical reasons (i.e. not social or domestic reasons), and
-
under the direct supervision of a specialist
Mental health treatment delivered at home or in the community is not covered by the scheme.
Back to topThe scheme is designed to cover consultations, diagnostics and treatment in the UK, and therefore provides limited cover whilst abroad. We strongly recommend that you have adequate travel insurance and / or a European Health Insurance Card / Global Health Insurance Card in place before you travel abroad.
If you wish to claim for emergency treatment received abroad, you must send us proof of how long you were abroad for (this period should not exceed 28 consecutive days). You should also send us all medical bills and receipts associated with this. Failure to submit receipts within six months of your treatment date may result in the claim being denied.
We will reimburse reasonable and customary costs for overseas emergency treatment as outlined below:
| Benefit | Reimbursement level |
| Specialist fees | Within our reasonable and customary fees |
| MRI, CT and PET scans |
Up to £100 per trip |
| Outpatient surgical procedures | Up to £100 per trip |
| Other emergency outpatient consultations, diagnostics or treatment (excluding MRI, CT and PET scans, and outpatient surgical procedures) | Up to annual outpatient benefit limits, as outlined in your table of benefits |
| Inpatient or day case surgical procedures | Up to £200 per trip |
We will only pay up to the above limits if the following apply to your consultations, diagnostics or treatment:
-
it is eligible for benefit, and
-
it is carried out by a specialist who is:
-
fully trained and legally qualified and permitted to practice by the relevant authorities in the country in which this takes place, and
-
is recognised by the relevant authorities in that country as having specialised knowledge of, or expertise in, diagnosis / treatment of the disease, illness or injury being treated, and
-
the treating facility is specifically recognised or registered under the laws of the territory in which it stands for providing the care delivered, and
- the costs are covered under your scheme.
We will not pay for overseas emergency treatment in any country if:
-
the Foreign and Commonwealth Office has advised against travel to that country or area. If you are already in the country or area when the Foreign and Commonwealth Office advises against travel, and you require consultations, diagnostics or treatment, this should be claimed for under your travel insurance policy
-
you are already in that particular country or area and have been advised to leave unless prior written authority has been received from us. If you are unable to leave a particular country or area after being advised to do so, and you require consultations, diagnostics or treatment, this should be claimed for under your travel insurance policy
-
you travelled abroad despite being given medical advice not to travel abroad
-
you travelled abroad to for the consultations, diagnostics or treatment, or
-
the consultations, diagnostics or treatment you require are related to a pre-existing condition.
The scheme will not pay for:
-
GP services or fees
-
outpatient prescriptions
-
take home drugs and dressings
-
any costs associated with an evacuation or repatriation
-
any consultations, diagnostics or treatment that should be free or provided at a reduced cost under a reciprocal agreement or EHIC / GHIC.
Costs of private consultations, diagnostics or treatment in facilities in the European Union, Iceland, Liechtenstein, Norway or Switzerland or costs in state facilities in these countries which should have been free or reduced if you had had a European Health Insurance Card / Global Health Insurance Card are not covered under the scheme.
If you are a UK resident, you are entitled to medical assistance that becomes necessary, at reduced cost or sometimes free, when temporarily visiting a European Union (EU) country, Iceland, Liechtenstein, Norway or Switzerland. Only consultations, diagnostics or treatment provided under the state scheme (the country’s equivalent to the NHS) are covered. However, to obtain this you will need to take a European Health Insurance Card (EHIC) or Global Health Insurance Card (GHIC) with you.
EHIC are still valid if in date, but they have now been replaced by the GHIC. You can apply for a GHIC by clicking here.
The scheme will not cover you for the costs of an evacuation or repatriation should you require this. Therefore we strongly recommend that you take out appropriate travel insurance if you are going abroad to ensure that you have adequate cover for any healthcare needs you have along with cover for loss of luggage etc.
Back to topCancer cover explained
We know that a cancer diagnosis can be a life changing event. Therefore we have provided a specific section within your scheme to help you understand the level of cover available to you for cancer treatment.
The scheme provides benefit for eligible outpatient, day case and inpatient treatment for cancer. To ensure that you receive the highest quality of care at all times we identify centres of excellence for the treatment of cancer. If you are diagnosed with cancer we may require you to transfer to one of these centres. These centres may be in either the private or NHS sector.
Should you choose to receive free eligible inpatient, day case or outpatient treatment at an NHS centre you may be eligible for the NHS cancer cash benefit as shown on your table of benefits.
One of our nurse case managers will be able to provide information on the treatment options available to you and support you through your treatment.
The table below provides a summary of the cancer cover available and should be read alongside your table of benefits.
| Summary of cancer benefits | What’s covered | What’s not covered |
| Where will I be covered to have treatment? |
You will be covered in full for eligible treatment:
|
You will not be covered for:
|
| What diagnostic tests will I be covered for? |
You will be covered in full for:
|
You will not be covered for any diagnostic tests that are:
|
| Will I be covered for surgery? |
You will be covered in full for:
|
You will not be covered for surgery that is:
|
|
Will I be covered for preventative treatment? |
You will be covered for prophylactic (preventative) surgery if:
For example, we will pay for a mastectomy to a healthy breast in the event that you have been diagnosed with cancer in the other breast and your specialist indicates that prophylactic surgery is medically necessary and will be carried at the same time as surgery to the diseased breast. You must have our written agreement before you have tests, procedures or treatment and we will need full clinical details from your specialist before we can give our decision. |
You will not be covered for any preventative treatment, including:
|
|
What drug treatments will I be covered for? |
You will be covered in full for:
Where treatment is for a secondary or metastatic cancer, cover will be available for the first line of drug treatment only. |
You will not be covered for:
|
| Will I be covered for radiotherapy? |
You will be covered in full for radiotherapy, including when given for pain relief. |
You will not be covered for radiotherapy that is:
|
| Will I be covered for end of life care? |
|
You will not be covered for:
|
|
What cover will be available for routine monitoring when |
You will be covered for follow-up tests and specialist consultations to monitor you for a maximum of ten years from the date you complete treatment for cancer. |
|
|
What other benefits and services are available? |
You will be covered for:
Please note that these are subject to any limits as detailed in your table of benefits. You will also be covered for the cost of mastectomy bras and wigs as detailed in your table of benefits. |
You will not be covered for:
|
|
Are there any other supportive benefits available? |
You also have access to a comprehensive support platform delivered by Perci Health to provide you with additional support for the psychological, physical and practical impacts of cancer when it is needed most. For further information please see the your cancer support explained page. |
|
Your cancer support explained
We know that a cancer diagnosis can be a life changing event and we are committed to supporting you in the event that you are impacted by cancer. This is why we have partnered with Perci Health to provide you with additional support for the psychological, physical and practical impacts of cancer.
Perci are able to offer you support regardless of how you have been impacted by cancer
- Are you receiving active treatment for a cancer diagnosis?
- Are you looking for some additional support following completion of your cancer treatment?
- Are you caring for a loved one with cancer?
Regardless of your situation, Perci are able to provide a personalised care plan, a dedicated cancer nurse, and access to caring cancer experts from over 20 different support types to help reduce the impact of cancer.
| Recovery and rehabilitation | Symptom management | Support for carers |
|
|
|
Access to this service will not be subject to an excess, scheme underwriting or any healthcare scheme benefit limits, if any apply.
Please note; this benefit is available to members over the age of 18.
For further information and to get started access the ‘your cancer support’ tile on the Member Zone or via the My Healix app.
Further - Precision Cancer Service
We know that a cancer diagnosis can be life-changing, and we’re here to support you every step of the way. That’s why we’ve partnered with Further to offer the Precision Cancer Service, giving you access to advanced genetic testing and expert advice to help guide your treatment.
The Precision Cancer Service is designed to support you in the event of an advanced or complex cancer diagnosis. The following cancers are eligible for this service:
· Cancers that haven’t responded to initial treatment (as confirmed by your oncologist)
· Advanced-stage cancers (stage III or IV)
· Cancers where the original site isn’t clear (cancer of unknown primary)
· Rare cancers.
If you are diagnosed with an eligible cancer, the Precision Cancer Service provides comprehensive genetic testing, known as a Somatic test.
These somatic tests are reviewed by world-leading experts who will provide a personalised report with treatment recommendations.
The service will also offer a complementary germline test if a hereditary risk is suspected in your case. If a hereditary cancer risk is identified through germline testing, Further can arrange the same test for your biological children (and, in some cases, siblings) to determine if they might also be at risk.
If a clinical trial might be right for you, Further can also help you find one.
Please note:
· some types of cancer may not be eligible for the service, depending on your scheme and any personal or scheme exclusions
· cover for any treatment recommendations presented by this service will be subject to all scheme terms and conditions, including but not limited to, scheme exclusions and monetary limits where applicable
Our nurse case managers are here to guide you through your cancer treatment and provide information on your available options.
Fertility treatment explained
We know that fertility concerns can have a major impact on life so we have developed a benefit to offer support and assistance when it matters most.
One of our experienced claims team will be able to provide information on the treatment options available to you and support you through your treatment.
The table below provides a summary of the cover available and should be read alongside your table of benefits.
The following benefits are only eligible for individuals who are covered by the healthcare scheme and are under the age of 43.
| Summary of benefits | What is covered |
|
Who can receive treatment? |
You will be covered within the benefit limit for fertility treatment providing you are a member of the healthcare scheme and under the age of 43 years. You must be under the age of 43 at the beginning of each individual treatment cycle. Should you turn 43 during treatment, cover will be available up to the end of the current treatment cycle only. |
|
When is cover eligible from? |
You will be covered within the benefit limit for ART after completion of a 12 month waiting period which starts from the date you join the healthcare scheme. |
|
Where am I covered to receive treatment? |
You will be covered within the benefit limit for treatment in the UK at a facility approved for use and licensed by the HFEA (Human Fertilisation and Embryology Authority). |
|
What treatments am I covered for? |
You will be covered within the benefit limit for surgery for the following conditions where this is affecting your fertility and is recommended by a specialist:
You will be covered within the benefit limit for eligible assisted reproductive technology (ART) treatment including:
These treatments will be eligible for cover where treatment has been recommended by a specialist. You will also be covered for:
Most fertility treatment costs are attributed to the female. As a male claimant you will be eligible for the following treatment:
Most fertility treatment costs are attributed to the female. As a male claimant you will be eligible for the following:
|
|
Am I covered for surgical sperm extraction? |
You will be covered within the benefit limit for the costs associated with surgical sperm extraction when medically necessary and recommended by a specialist. |
|
How many cycles of IVF / IUI am I covered for? |
You will be covered within the benefit limit for repeated cycles of IUI / IVF / ICSI / FET. |
|
Am I covered for the genetic testing of eggs / sperm / embryos? |
You will not be covered for any costs associated with genetic testing (including, but not limited to, karyotype testing or pre implantation genetic testing). |
|
Am I covered for sperm washing? |
You will not be covered for the cost of sperm washing to prevent blood borne viruses from being transmitted. |
|
Am I covered for the cost of take home drugs |
You will be covered within the benefit limit for the cost of fertility medications required for the purpose of providing the fertility treatment and prescribed by your specialist as part Cover is available for the following:
Cover is not available for:
Following confirmation of a viable pregnancy, the cost of any further medication required to maintain the pregnancy will not be eligible for benefit. |
|
Am I covered for donor insemination / donor eggs? |
You will not be covered for the cost of donor eggs or sperm required to achieve a pregnancy. |
|
Am I covered for the costs of surrogacy? |
You will not be covered for the costs of ART with the use of a surrogate. |
|
Am I covered for the cost of freezing resultant embryos following IVF treatment? |
You will be covered within the benefit limit for the costs of embryo freezing for a total of 12 months following a cycle of IVF – after which time any further costs associated with the continued storage of embryos will no longer be eligible for cover. |
|
When does cover end? |
Cover for ART will end at the point that a viable pregnancy is confirmed by ultrasound scan or when the benefit limit has been reached, whichever is reached soonest. Once a pregnancy has been confirmed, any further scans or pregnancy related treatment will need to be taken on the NHS and the pregnancy exclusion would apply. |
|
Am I covered for treatment ‘add ons’ recommended by the clinic? |
You will be covered within the benefit limit for the cost of treatment ‘add ons’ only where there is adequate evidence as to their effectiveness as defined by the HFEA. |
|
Am I covered to freeze my eggs / sperm to use at a later time in life? |
You will not be covered for the cost of egg or sperm freezing in order to preserve fertility for use at a later time in life. |
|
Are same sex couples and individuals not in a partnership eligible for ART? |
You will be covered within the benefit limit for treatment recommended by a specialist, however, the costs of the associated donor sperm or eggs required to achieve a pregnancy will not be eligible for cover. |
|
Can I continue treatment that I started through self-pay prior to joining the healthcare scheme? |
You will be covered within the benefit limit for the continuation of eligible pre-paid treatment. Treatment costs already incurred prior to the benefit being eligible will not be reimbursed. |
|
Am I covered for reversal of sterilisation to correct infertility? |
You will not be covered for the cost of sterilisation reversal where this is the cause of infertility in either partner. |
|
Am I covered for complementary therapies related to fertility? |
You will be covered for complementary therapies as detailed in your table of benefits. |
|
Am I covered for counselling or mental health treatment related to my infertility? |
You will be covered for mental health treatment as detailed in your table of benefits. |
|
Am I covered for multi-cycle treatment packages? |
You will be covered within the benefit limit for the cost of single cycle treatment only. We are unable to cover ‘multi-cycle package’ costs that may not be used. |
|
Do I need to self-pay for treatment |
You may be required to self-pay for fertility treatment at a clinic where they are unable to accept payment from us. Eligible fertility treatment can then be reimbursed as long as this is requested within 6 months of the treatment date. Reimbursement can only be made after the fertility treatment has taken place. |
Gender dysphoria explained
We know that gender dysphoria can cause distress and discomfort for individuals who don't identify with the gender or sex they were assigned at birth. Therefore, we have provided a specific section within your scheme to help you understand the level of cover available to you should you experience this.
This table provides a summary of the cover available and should be read alongside your table of benefits.
Cover for gender dysphoria is available for members over the age of 18 years within the benefit limit of £10,000 per member per scheme lifetime
For help and support, please contact the claims helpline.
| Summary of benefits | What’s covered | What’s not covered |
| Where will I be covered to have treatment? |
You will be covered within the benefit limit for
|
You will not be covered for:
|
| What will I be covered for? |
You will be covered within the benefit limit for
|
You will not be covered for:
|
| What other benefits and services are available? |
You will be covered within the benefit limit for:
|
You will not be covered for:
|
Overseas emergency repatriation and evacuation
The scheme benefits generally only apply when you have treatment in the UK, and as a result, there is no coverage for treatment outside of the UK. For this reason we strongly advise you to take out travel insurance when travelling abroad.
However, In the event that you should fall ill abroad your healthcare scheme does provide access to an overseas assistance company line, which is provided by Healix International.
This line is manned 24/7 to provide help and assistance in any part of the world. This service can provide immediate advice and may be able to arrange to put you in touch with an English-speaking doctor where available. They will be able to offer support and advice to ensure that the treatment you are receiving is medically appropriate and of a satisfactory standard.
Please note that, whilst the costs of using the overseas assistance company line is covered by your healthcare scheme, any costs for overseas appointments or treatment will not be paid for by the scheme and will be your liability if you do not have alternative cover in place.
In the event that an emergency repatriation is requested and the overseas assistance company are in agreement that this is medically necessary, cover will be available as detailed below.
You must advise us of any cover held with a travel insurance policy. The scheme shall, at its own expense, reserve the right to speak with the other insurer in any way considered appropriate in your name. You must co-operate with all reasonable requests in this respect.
Contact the overseas assistance company line quoting 'HHS'
Tel: +44 (0) 203 8231 322
E-mail: hhsrepat@healix.com
| Summary of benefits | What is covered? |
|
What if I need evacuating or repatriating back to the UK? |
In the event of an emergency the scheme may also provide an emergency evacuation and repatriation service. This service is available if you should fall ill abroad and the treatment you require either not be available locally or the local medical facilities not be of an acceptable standard in the opinion of the overseas assistance company. The overseas assistance company will arrange to repatriate you by air ambulance, scheduled airline service or any other medically appropriate transport including qualified medical escort(s) where medically necessary. The evacuation and repatriation service will arrange you to be returned to the UK only. Any costs for treatment prior to an emergency evacuation and repatriation will not be paid for by the scheme. |
|
When am I not covered for evacuation or repatriation, including the repatriation of mortal remains? |
This service is not available for cover in the following circumstances:
|
|
What happens when I return to the UK? |
On arrival back to the UK, cover for private treatment will be assessed according to the general terms and conditions of your healthcare scheme. Treatment should be taken on the NHS, until cover has been confirmed, to prevent you incurring any unwanted costs. |
|
What costs are covered for evacuation and /or repatriation |
You will be covered in full for any medical and transportation expenses arranged by and charged by the overseas assistance company to bring you back to the UK. |
|
Will my family be covered to travel with me? |
You will be covered for:
|
|
What costs are not covered during an evacuation or repatriation |
You, and any eligible accompanying person will not be covered for :
|
|
What happens in the event of my death overseas? |
You will be covered for the costs associated with the repatriation of your mortal remains back to the UK. This will only be covered when the transport is required for the repatriation of mortal remains and is arranged via the overseas assistance company. |
|
Who do I contact to arrange an evacuation / repatriation? |
In the event that an evacuation or repatriation is required, please contact the overseas assistance company line on the number detailed above and they will be able to advise you on the cover available and, where eligible, make the necessary arrangements. |
Second medical opinion
Should you decide that you would like to receive a second medical opinion to ensure you are fully confident with your specialists recommendations please contact us on the claims helpline to discuss pre-authorisation. Our experienced claims team will be able to advise and support you through this process.
Second medical opinions will be arranged with a specialist who is an expert in their field and is recognised for the purposes of providing such second opinions. Without written authorisation for a second opinion, payment cannot be made for any recommended or resulting treatment.
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <
Treatment
Treatments
Trust Deed
Trustee, Trustees
United Kingdom
Waiting Period
We, Us, Our
You, Your
Gender Dysphoria
Gender Incongruence
High risk activities
Scheme
Pandemic
Epidemic
Neurodevelopmental disorders
Member Zone
Women's health services
At Healix, we know it’s vital to receive quick access to healthcare, we have therefore made access to women’s health services as easy and smooth as possible.
You can contact the claims helpline, and speak to our experienced claims team, they will be able to guide you to the most appropriate services, including access to a remote advice service with a gynaecologist.
The majority of women’s health conditions would be covered under your normal outpatient and inpatient benefits, however some conditions would traditionally sit outside the healthcare scheme cover. We have therefore created the additional Women’s health benefits, to provide some extra cover, if this is required. Our experienced claims team will be able to advise you further on whether your condition and treatment would be covered under these extra benefits.
The below table outlines the services available, and how to access them through your healthcare scheme.
| Women’s health concern | How to access treatment |
|
For advice regarding any general women’s health query, including, but not limited to, menopause symptoms or contraception advice |
You may self-refer by contacting the claims helpline, without the need for a GP referral, and we will be able to direct you to the most appropriate service available to you. This includes access to remote consultations and diagnostic tests, with our in-network specialist gynaecologists (where appropriate). Cover is available up to the limits specified in your table of benefits. Once this benefit limit has been reached, the scheme rules apply as detailed in your exclusions and limitations. |
|
If you are concerned about a breast abnormality, for example a lump |
Contact the claims helpline to speak to our claims team, who will be able to support you and direct you to the most appropriate specialist, without the need to see your GP first. Cover will be available as specified in your table of benefits. Further information about early signs of cancers and self-referral can be found here. |
|
If your GP has referred you to a specialist gynaecologist, for example, for unusual bleeding |
Contact the claims helpline to speak to our experienced claims team, who will be able to open a new claim. The claims team will also be able to direct you to the most suitable specialist. |
|
If your GP has referred you for fertility investigations |
Contact the claims helpline to speak to our experienced claims team, who will be able to open a new claim. Cover will be available from your fertility investigations benefit, as specified on your table of benefits. |
|
If you are experiencing complications of pregnancy |
Contact the claims helpline to speak to our experienced claims team, who will be able to advise if there is any cover available for you. Cover will be available for specific pregnancy complications only, as specified in your table of benefits. |
|
For physiotherapy treatment for a pelvic problem such as stress incontinence |
Contact the claims helpline, without the need for a GP referral, and speak to our experienced claims team who will arrange a telephone based assessment with a senior physiotherapist, to determine the most appropriate treatment for you. Cover is available from your physiotherapy benefit, as specified in your table of benefits. |
Men's health services
At Healix, we know it’s vital to receive quick access to healthcare, we have therefore made access to men’s health services as easy and smooth as possible.
You can contact the claims helpline, and speak to our experienced claims team, they will be able to guide you to the most appropriate services, including access to a remote advice service with a men’s health specialist.
The majority of men’s health conditions would be covered under your normal outpatient and inpatient benefits, however some conditions would traditionally sit outside the healthcare scheme cover. We have therefore created the additional men’s health benefits, to provide some extra cover, if this is required. Our experienced claims team will be able to advise you further on whether your condition and treatment would be covered under these extra benefits.
The below table outlines the services available, and how to access them through your healthcare scheme.
| Men’s health concern | How to access treatment |
|
For advice regarding any general men’s health query, including urinary symptoms, sexual health and fertility advice |
You may self-refer by contacting the claims helpline without the need for a GP referral and we will be able to direct you to the most appropriate services available to you. This includes access to remote consultations and diagnostic tests with our in-network men’s health specialists (where appropriate). Cover is available up to the limits specified in your table of benefits. Once this benefit limit has been reached the scheme rules apply as detailed in your exclusions and limitations. |
|
If you are concerned about early signs of prostate or testicular cancer |
Contact the claims helpline to speak to a nurse case manager who will be able to support you and direct you to the most appropriate specialist without the need for seeing your GP first. Cover will be available as specified in your table of benefits. Further information about early signs of cancers and self-referral can be found here. |
|
If your GP has referred you to a specialist |
Contact the claims helpline or access the claims portal to open a new claim. Cover will be available as specified in your table of benefits. One of our experienced claims team will be able to direct you to the most suitable specialist. |
|
If your GP has referred you for fertility investigations |
Contact the claims helpline to speak to our experienced claims team, who will be able to open a new claim. Cover will be available from your fertility investigations benefit, as specified on your table of benefits. |
|
For physiotherapy treatment for a pelvic problem such as stress incontinence |
Contact the claims helpline, without the need for a GP referral, and speak to our experienced claims team who will arrange a telephone based assessment with a senior physiotherapist, to determine the most appropriate treatment for you. Cover is available from your physiotherapy benefit, as specified in your table of benefits. |
Self-referred cancer benefits
Experiencing symptoms that can be associated with cancer can be concerning. It's important to remember that these symptoms are not definitive of cancer but may indicate a risk. We are here to support you in obtaining timely investigations for any symptoms that could potentially be related to cancer.
If you experience any of the symptoms listed below then you are able to call and speak directly to our claims team to self-refer for a consultation and diagnostic tests.
This means that you no longer need to see your GP before accessing private treatment for these concerns in order to prevent any delays in reaching a diagnosis.
If you are experiencing any of the symptoms below, call the claims helpline and our experienced claims team will be able to help direct you into one of our robust clinical pathways with our in-network providers to help reach a diagnosis.
| Type of cancer | Signs and symptoms to watch out for |
|
Breast cancer |
|
|
Bowel cancer |
|
|
Prostate cancer |
Raised PSA level as specified below:
|
|
Testicular cancer |
|
|
Skin cancer |
Any of the following changes to a mole or lesion on the skin:
|
Please remember that these signs are also features of common health problems that
are not caused by cancer, such as a cyst, piles or infection.
In the event that a cancer diagnosis is made, cover will be available as detailed in your cancer cover explained and one of our nurse case managers will support you and be able to provide information on the treatment options available to you.
Please contact us via the Member Zone, the My Healix app or by calling the claims helpline to get further advice and to open a new claim. As with all of your healthcare benefits it is important that you obtain pre-authorisation before receiving any treatment to ensure your claim is eligible and to prevent you incurring any unwanted costs.
Musculoskeletal health pathway
Musculoskeletal conditions affect your muscles, bones and joints. They are very common and tend to increase with age.
Pain and discomfort can affect your daily activities but early diagnosis and treatment may help to ease your symptoms and improve the length of time it takes to recover. We have designed the Healix musculoskeletal pathway with this in mind.
How to make a claim
As soon as you experience bone or joint pain you can use our digital physiotherapy triage service. The service is available to all members over the age of 16.
This can be accessed via the Member Zone or the My Healix app where you will be directed straight through to begin your online journey and treatment pathway without the need to contact the claims helpline.
Click here to access the Member Zone using your individual member number
This digital service is designed to provide an assessment of your needs and guide you to the best course of treatment.
Where self-managed care is appropriate, you are able to immediately access a tailored exercise programme with in-app access to a clinician as required. If needed, you will be guided to face-to-face physiotherapy treatment with our network provider.
If face to face physiotherapy sessions are recommended these will not be subject to an excess, scheme underwriting or any scheme limits (if these apply) when treatment is taken with our digital treatment pathway provider. All other healthcare scheme terms and conditions will apply.
Telephone assessment
If you are unable to access the Member Zone or the My Healix app, call the claims helpline to arrange a telephone based clinical assessment. Our experienced team will take your details and arrange for you to have an initial telephone consultation with a physiotherapist at a convenient time for you who will recommend the most appropriate treatment.
The telephone-based clinical assessment will not be subject to any excess, if one applies, however it will be applied to face-to-face treatment should this be required. All other healthcare scheme terms and conditions will apply.
Mental health pathway
The importance of mental health and wellbeing is becoming increasingly recognised in today’s busy world. Acknowledging stress and anxiety then seeking help are the first steps to developing coping strategies and recovery.
If you are experiencing stress, anxiety or depression or any other mental health problem, please refer to the below for further information on how your scheme can support you.
How to make a claim
Members are able to access a digital emotional wellness triage and immediate advice via the Member Zone or the My Healix app. The service is available for everyone over the age of 16.
Click here to access the Member Zone using your individual member number
| Benefits | What is available? | What can you use this for? |
| Digital emotional wellness triage |
|
|
If face to face mental health treatment is recommended you will be directed into an initial episode of treatment with our network provider.
Where face to face mental health treatment takes place, this will not be subject to an excess, scheme underwriting or any scheme limits (if these apply) when treatment is taken with our digital treatment pathway provider.
Should additional sessions be required beyond the initial episode of treatment, all healthcare scheme terms and conditions, including excess, will then apply.
Telephone assessment
Should you be unable to access the Member Zone or the My Healix app, you can contact the claims helpline for support and advice. There is no need to see your GP or obtain a referral letter unless you are under the age of 18.
Our experienced claims team will take your details and arrange for you to have an initial telephone consultation with a senior psychological therapist at a convenient time for you. This will give you an opportunity to talk through your concerns and agree on the best treatment pathway.
This could be one of several options including:
-
face to face cognitive behavioural therapy (CBT)
-
guided online CBT
-
counselling
-
referral onwards to see a psychiatrist
Healix will pre-authorise your assessment and treatment (within benefit limits where applicable) and settle all invoices directly.
The telephone-based clinical assessment will not be subject to any excess, if one applies, however it will be applied to face-to-face treatment should this be required. All other healthcare scheme terms and conditions will apply.
*Under 18s will require a referral letter from a GP or specialist.
Digital skin pathway
Changes in your skin can be concerning, though most are not cancer-related. Our digital skin pathway ensures rapid assessment and results, with recommendations for further consultations, diagnostics and treatment as needed, depending on your diagnosis. Any subsequent cover will be subject to the healthcare scheme terms and conditions.
This pathway is suitable for a variety of skin conditions, and our experienced claims team can guide you to the most appropriate pathway based on your symptoms.
The table below outlines the skin complaints best suited for referral into our digital skin pathway.
| Skin conditions suitable for the skin pathway | Skin conditions not suitable for the skin pathway |
|
|
How to access the digital skin pathway
Our digital skin pathway is designed to be simple and efficient. Follow the steps below to access fast, expert care:
Please note, face-to-face consultations with dermatologists within our network will not be subject to our reasonable and customary fees. If you choose see a specialist outside our network, these fees will apply.
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <
Treatment
Treatments
Trust Deed
Trustee, Trustees
United Kingdom
Waiting Period
We, Us, Our
You, Your
Gender Dysphoria
Gender Incongruence
High risk activities
Scheme
Pandemic
Epidemic
Neurodevelopmental disorders
Member Zone
Employee Assistance Program (EAP)
Diageo employees have access to an Employee Assistance Programme (EAP) tlk2 through Workplace Options. You will need to register your account before using the service
Please find the access details below, including your login details; please have this ready when accessing the service.
- Access:
- App - search iConnectYou in your Google Play or App Store
- Website - https://www.workplaceoptions.com/ie/
- Username: Diageo
- Password: employee
- Telephone number: 0208 987 6230
This service is not provided through Healix. Should you have any queries, please contact Workplace Options on 0800 328 8597 or via email support@resourcesforyourlife.com
Virtual GP
Diageo members have access to a virtual GP service called Spark, provided by Spectrum.Life.
Details on how to access this service and how to register for an account (if required) are listed below; please have this ready when accessing the service.
- How to access: Search for Spectrum.Life in Google Play or the App Store
- Webpage: https://landg.spectrum.life/login
- Company code: G00710230
- Telephone Number: 0330 818 0006
This service is not provided through Healix. For any queries, please contact Spectrum.Life or the Diageo team.
If Spectrum.Life make an onward referral, we can accept this in place of a referral from your NHS GP, provided that their recommendation is eligible. Contact us to confirm eligibility.
Onward referrals are subject to your scheme underwriting, any personal exclusions and scheme exclusions and limitations. If additional information about your medical history is needed, we may require your consent to contact your NHS GP.
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <
Treatment
Treatments
Trust Deed
Trustee, Trustees
United Kingdom
Waiting Period
We, Us, Our
You, Your
Gender Dysphoria
Gender Incongruence
High risk activities
Scheme
Pandemic
Epidemic
Neurodevelopmental disorders
Member Zone
Making a claim
Register your claim using our My Healix app or Member Zone. Alternatively, you can call the claims helpline to confirm if cover is available.
In order for us to accurately assess cover under the terms and conditions of your scheme, we may ask to see a copy of your GP referral letter when you open a new claim.
Always contact the claims team before arranging or receiving any treatment.
Access the Member Zone
Click here to access the Member Zone using your individual member number
Call the claims helpline:
0208 608 4022
Monday-Friday 08.00-19.00 (Excl. bank holidays)
Saturday 09.00-13.00
We will confirm:
-
whether your proposed treatment is eligible for cover under the scheme
-
whether your proposed treatment costs will be covered under the scheme
-
any benefit limits or excess that may apply to your claim
To help you make the best possible use of the scheme, we have provided you with a how to claim summary
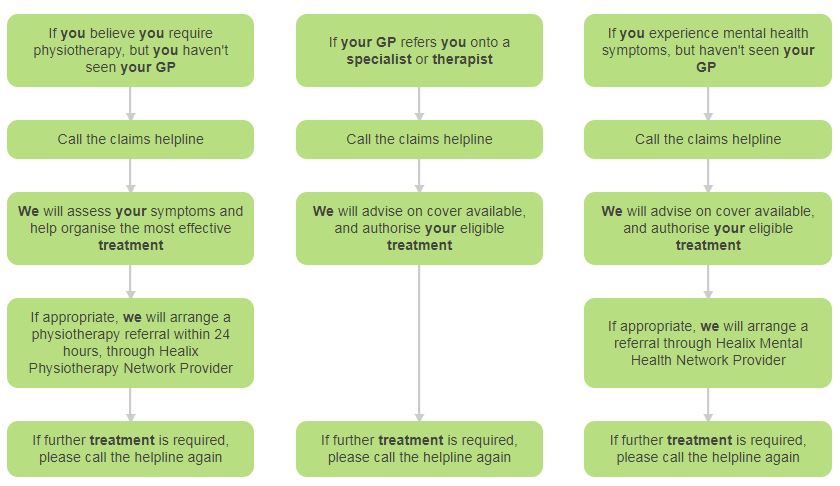
How to claim summary
If you believe you require physiotherapy, but you haven't seen your GP
If your GP refers you onto a specialist or therapist
If you experience mental health symptoms, but haven't seen your GP
Log your claim via the Member Zone, the My Healix app or call the claims helpline
Log your claim via the Member Zone, the My Healix app or call the claims helpline
Log your claim via the Member Zone, the My Healix app or call the claims helpline
We will assess your symptoms and help organise the most effective treatment
We will advise on cover available, and authorise your eligible treatment
We will advise on cover available, and authorise your eligible treatment
If appropriate, we will arrange a physiotherapy referral within 24 hours, through Healix Physiotherapy Network Provider
If appropriate, we will arrange a referral through Healix Mental Health Network Provider
If further treatment is required, please visit the Member Zone, the My Healix app or call the helpline again
If further treatment is required, please visit the Member Zone, the My Healix app or call the helpline again
If further treatment is required, please visit the Member Zone, the My Healix app or call the helpline again
Your scheme underwriting
Medical History Disregarded (MHD)
We will not apply any personal medical exclusions to your scheme. However your eligibility for cover will be subject to the general terms of the scheme. Please refer to exclusions and limitations for further information.
Your excess
Per scheme year excess
All members are liable for an excess of £100, payable once per scheme year if you make an eligible claim.
The excess will be applied to the first eligible treatment you receive in each scheme year, regardless of when the last excess payment was made. This applies whether the treatment is for the same condition, a related condition, or for an entirely new condition.
To ensure clarity, contact us before receiving any treatment (including consultations, diagnostics or therapies) to confirm when the excess will apply.
Reasonable and customary fees
We apply a schedule of reasonable and customary (R&C) fees for charges made by providers, including but not limited to, a specialist, practitioner, physiotherapist, complementary practitioner or a psychological therapist. These fees are aligned with the common codes and principles set out by the Clinical Classification and Schedule Development (CCSD) group. Our fee levels are carefully reviewed, based on what the majority of providers charge for medical and surgical services, and are validated by our clinical support team, and panel of specialist advisors.
If you choose a provider who charges above our fee schedule, you have the option to either pay the difference yourself or we can help identify an alternative provider who charges within the approved fee schedule.
Refer to our fee schedule or contact us for further information.
Hospital cover
Open network
We have an open network which means you are able to attend the hospital of your choice. Please note reasonable and customary charges will apply to specialists at all hospitals. For help in finding a hospital, please refer to our hospital finder.
What happens in an emergency?
Most private hospitals are not set up to receive emergency admissions. In the event of an emergency you should:
- call for an NHS ambulance
- visit the accident and emergency department at the local NHS hospital
If you would like to be transferred to a private facility, please contact the claims helpline. We will then be able to confirm whether your proposed treatment is eligible under the healthcare scheme. Please note you must contact us before you transfer to a private facility.
You will not be covered for:
- the cost of emergency treatment in a private walk-in centre, accident and emergency department or clinic
- the cost of treatment in an intensive care or high dependency unit if you have been transferred specifically to receive this care
- the costs of the transfer to a private facility specifically to receive treatment in an intensive care or high dependency unit
Exclusions and limitations
The following are conditions and treatments which are not covered under your scheme. If you are unsure about anything in this section, please contact the claims helpline.
Exclusions and limitations
We do not pay for treatment to relieve symptoms commonly associated with or caused by ageing, puberty or other natural physiological cause.
Please note: we will pay for remote consultations and diagnostics related to women’s or men's health concerns with a specialist gynaecologist or men's health specialist as specified in your table of benefits.
We do not cover any consultations, diagnostics or treatment required for alcohol, solvent or drug abuse, or any treatment arising from such abuse or addiction. This includes mental health treatment.
Exception: we cover one addiction treatment programme for alcohol, solvent or drug abuse per scheme lifetime under the inpatient mental health benefit, as detailed in your table of benefits.
We do not cover any consultations, diagnostics or treatment to desensitise or neutralise any allergic
condition or disorder.
We do not pay for the supply or fitting of appliances, physical aids or devices (including but not limited to hearing aids, spectacles, contact lenses, external prostheses and orthotics etc) which do not fall within our definition of a surgical appliance other than as listed in your table of benefits. Any consultations relating to these are also not covered.
We do not pay for:
• contraception or any consequence of using contraception
• sterilisation and/or reversal
Please note: we will pay for remote consultations and diagnostics related to women’s or men's health concerns with a specialist gynaecologist or men's health specialist as specified in your table of benefits.
We do not cover any consultations, diagnostics or treatment related to chronic conditions that require ongoing care. A chronic condition is defined as a medical condition with at least one of the following characteristics:
- requires ongoing or long-term monitoring through consultations, examinations, check-ups and / or tests
- needs ongoing or long-term control or relief of symptoms
- requires rehabilitation or for you to be specially trained to cope with it
- continues indefinitely
- has no known cure, or
- comes back or is likely to come back.
This will apply to all medical conditions, whether or not a diagnosis has been made.
Exception: we cover acute eligible treatment (including consultations, diagnostics and therapies) arising out of a chronic condition, or treatment of acute symptoms of a chronic condition that flare-up. Such treatment will only be covered if it is likely to lead quickly to a complete recovery, or to you being fully restored to your previous state of health without you having to this long-term. For example, we pay for treatment following a heart attack which is the result of chronic heart disease. This exception does not apply to mental health conditions.
In some cases, it may not be immediately clear that the disease, illness or injury being treated is a chronic condition. In such situations, even if we have previously paid for treatment, we are not obliged to cover the ongoing costs of continuing, or similar, treatment.
This exclusion does not apply to cancer treatment.
Exception: we cover consultations, diagnostics and treatment of chronic conditions as outlined in your table of benefits.
We do not pay for treatment which arises from, or is related to any exclusion listed in this guide or treatment which arises from or is related to a surgical procedure we do not cover.
We do not pay for treatment of any medical condition which is caused or contributed to by; nuclear, radioactive, biological or chemical contamination, war (whether declared or not), act of foreign enemy, riot, revolution, invasion, civil war, rebellion, insurrection, overthrow of a legally constituted government, explosions of war weapons, terrorist act or military activity. We will not pay for treatment of any medical condition which is received while you or your dependants are carrying out army, naval or air services duties.
We do not pay for treatment if it is primarily used for domestic and/or social reasons.
We do not pay for any treatment to change your appearance even when required for psychological reasons.
We do not pay for any treatment, including surgery:
-
where the intention of treatment, whether directly or indirectly, is the reduction or removal of healthy, surplus or fat tissue (for example, weight reduction surgery / treatment)
-
where the aim is to aesthetically enhance the appearance of the face or body where no functional condition is present (for example, botox, fillers or asymptomatic rhinoplasty)
Exception: we will pay for medically necessary treatment to restore your appearance in the following circumstances:
-
where it results from an eligible underlying disease process
-
following eligible treatment (including cancer treatment)
-
where the condition is causing a functional problem
Please note: we use clinical guidance as a benchmark for deciding whether the exceptions above are eligible for cover. All requests for cover must be submitted in writing with supporting medical information.
We do not pay for any dental or oral treatment other than as listed in the exception below.
Exception: we cover eligible treatment related to the following specified oral surgical operations only, when treatment is carried out by a specialist:
- surgical removal of a buried, infected or impacted tooth
- apicectomy or removal of the tip of a tooth’s root
- enucleation of a cyst of the jaw (removing a cyst from the jaw bone)
- surgical drainage of a fascial space abscess
- reimplantation of a natural tooth that has been knocked out or dislodged in an accident
- treatment of facial and mandibular fractures
We do not pay for treatment for or associated with dialysis.
We do not pay for drugs and dressings provided or prescribed for use as an outpatient or for you to take home, other than those outlined in the cancer cover explained page.
We do not pay for:
- emergency treatment or NHS cash benefit for treatment taken in a private or NHS walk-in centre, accident and emergency department or acute assessment unit or equivalent
- private surgical treatment or NHS cash benefit for surgical treatment when surgery is performed within 24 hours of an emergency admission
- private treatment or NHS cash benefit for treatment in an intensive care or high dependency unit if you have been transferred specifically to receive this care
- transferring to a private facility specifically to receive treatment in an intensive care or high dependency unit
We do not pay for treatments (including medication) which in our reasonable opinion are experimental or not yet approved by the National Institute for Health and Care Excellence (NICE), are being researched or lack sufficient evidence to conclude that:
- the harmful effects are outweighed by the beneficial effects
- they are likely to lead to the same or better outcomes than available alternatives
- they are based on established medical practice in the United Kingdom.
Examples of the criteria we use for considering a treatment as experimental include:
- the treatment is still undergoing clinical trials and/or yet to undergo a phase III clinical trial for the indication in question
- the treatment does not have approval from the relevant government body
- the treatment does not conform to usual clinical practice in the view of the majority of medical practitioners in the relevant field
- the treatment is being used in a way other than that previously studied or that for which it has been granted approval by the relevant government body
- the treatment is rarely used, novel, or unknown and there is a lack of authoritative evidence of safety and efficacy.
We do not pay for any treatment required for complications arising or resulting from experimental treatment that you receive or for any subsequent treatment you may need as a result of you undergoing any experimental treatment.
We do not pay for treatment to correct your eyesight due to long or short vision, including but not limited to, laser eye surgery, spectacles or contact lenses.
Exception: we will pay for eligible treatment to the eye resulting from an acute condition or injury.
We do not pay for the following unless specified in your table of benefits:
- any type of infertility investigations
- fertility treatment
- assisted reproduction, surrogacy, harvesting of donor eggs or donor insemination
- sperm collection and storage
- complications from any of the above
Please note: we will pay for remote advice consultations related to women’s or men’s health concerns with a specialist gynaecologist or men’s health specialist as specified in your table of benefits.
We do not pay for any treatment of gender dysphoria, or any treatment arising from or relating to gender dysphoria other than those listed in your table of benefits.
We do not pay for any GP consultations or visits other than those specified in your table of benefits. We do not pay for any charges for the completion of claim forms or referral letters, unless we have requested these specifically to assess your claim.
We do not pay for holistic or alternative medicine or therapies, unless these are specifically listed in your table of benefits. For example yoga, massage, spas and health resorts.
We do not pay for:
- any treatment caused by or resulting from you carrying out an illegal act
- any treatment resulting from a road accident where you were not wearing a seat belt (as required by law)
We do not pay for any treatment (following diagnosis) of adult or childhood neurodevelopmental disorders.
We do not pay for any fees or charges made by a healthcare provider for non attendance of appointments or late cancellation. This includes, but is not limited to, general practitioner visits, specialist appointments and / or therapy sessions.
We do not pay for any weight loss treatment including treatment required as a result of obesity.
We do not pay for treatment outside the United Kingdom including evacuation or repatriation, other than as specified in your table of benefits.
We do not pay for any costs of importing equipment into the United Kingdom or costs for any medical team to travel to the United Kingdom to treat you.
We do not pay for personal comfort and convenience items or services including but not limited to travel expenses, television, WIFI, telephone costs, newspapers, and guest meals.
We do not cover any consultations, diagnostics or treatment related to pregnancy or childbirth, other than as listed in the exception below.
Exception: we cover eligible treatment related to the following specified obstetric procedures / treatment:
- miscarriage or when the foetus has died and remains with the placenta in the womb
- still birth
- hydatidiform mole (abnormal cell growth in the womb)
- ectopic pregnancy (foetus growing outside the womb)
- post-partum haemorrhage (heavy bleeding in the hours and days immediately after childbirth)
- retained placental membrane (afterbirth left in the womb after the delivery of the baby)
- complications following any of the above conditions
- flare-up of non-pregnancy-related medical conditions that have been made worse by pregnancy
We will require full clinical details from your specialist to assess cover and eligibility.
We do not pay for any form of genetic testing or screening, health screening, health checks or preventative treatment, procedures or medical services where no disease is present.
We do not pay for treatment;
- recommended because of a genetic predisposition towards developing a medical condition
- recommended because of a family history of a medical condition
Please see cancer cover explained for information on preventative cancer treatment.
We do not pay for any treatment required due to sexual dysfunction, sexually transmitted infections or sexual problems, whatever the cause.
Please note: we will pay for remote consultations and diagnostics related to women’s or men's health concerns with a specialist gynaecologist or men's health specialist as specified in your table of benefits.
We do not pay for treatment for or relating to any speech disorder such as stammering. However we may pay for short term speech therapy for an acute condition immediately following eligible treatment. The speech therapy must be recommended by the specialist in charge of your treatment.
We do not cover consultations, diagnostics or treatment required as a consequence of injury sustained
whist training for, or participating in, sport for which you receive payment or sponsorship (other than travel
costs). Eligible treatment is aimed at restoring to your previous state of health; we do not cover treatment
aimed at enhancing performance in sporting activities.
We do not pay for any transplants, adoptive cell transfer, gene therapies and/or any complications related to, or resulting from these treatments. This includes, but is not limited to CAR T cell therapy, Tumour Infiltrating Lymphocyte therapy and stem cell/bone marrow treatments. We also do not pay for:
- donor costs
- harvesting
- storage
- administration
- and/or any complications/treatment arising from any of the above
Exception: we will pay for recipient costs for skin or corneal grafts when eligible for benefit
We do not cover any consultations, diagnostics or treatment that we do not consider to be medically necessary.
We do not pay for treatment carried out by a provider who we do not recognise as being qualified and/or registered to provide the type of treatment you need or for treating the medical condition you have.
We do not pay for treatment with sports therapists, massage therapists, or anyone who does not meet our definition of a practitioner or complementary practitioner.
We do not pay for any treatment carried out by you, your spouse, parents or children.
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <
Treatment
Treatments
Trust Deed
Trustee, Trustees
United Kingdom
Waiting Period
We, Us, Our
You, Your
Gender Dysphoria
Gender Incongruence
High risk activities
Scheme
Pandemic
Epidemic
Neurodevelopmental disorders
Member Zone
End of cover
Cover for you (the member) will end in the following situations:
-
if your employment with Diageo has come to an end for any reason
-
if you no longer live full time in the United Kingdom
-
if you pass away
-
if for any reason you or Diageo ask us to end cover
- if you or any of your dependants have given us misleading information, have kept something from us, or have broken the conditions of this scheme
If your cover ends, your dependants cover will also end on the same day as your cover.
Cover for dependants will end in the following situations:
Your partner's cover will end:
-
if you get divorced, or your civil partnership is dissolved. Cover for your partner will end as soon as the final decree/final dissolution order has been granted
-
if you no longer live together, then your partner will no longer be considered a dependant for the purposes of this scheme
Your dependant child’s cover will end:
-
after they have turned 25. They will be removed from cover on the next annual renewal date following their 25th birthday
-
if they get married, then they will no longer be considered a dependant for the purposes of this scheme
- if they no longer live full time in the United Kingdom
Employee's must inform their HR department as soon as possible of any changes of this matter.
If treatment has been authorised, but has not yet taken place, you will be responsible for any treatment costs if the scheme then terminates or you leave the scheme.
Continuation option
As Healix Health only provides corporate group schemes, we are unable to continue your cover as an individual if you leave The Diageo Healthcare Scheme.
We understand the importance of your healthcare and choosing a new provider may be daunting. We work closely with two providers to provide you with the best choice possible to take your healthcare forward.
What is a continuation option?
A continuation option allows members who resign or retire from an employer that provides workplace healthcare benefits to take out their own cover. You might be eligible to take over the benefits previously paid for by the employer, however it’s not always guaranteed that any ongoing claims will be covered.
National Friendly
Who are NF?
A Friendly Society that helps its members meet their health protection needs by offering you cover through private medical insurance policies.
How do I contact them?
Call 0333 014 6244, (8am-6pm Monday to Friday). Quote HEALIX and the team will be able to obtain the best possible terms for your transition.
What do they cover?
My Private Medical Insurance policy is a flexible product that offers cover for everyone up to age 85. You can choose between guided outpatient only cover all the way through to unlimited inpatient cover.
To find out more about National Friendly visit here.
Usay Compare
Who are Usay?
The largest individual health insurance intermediary and are experts at finding the best cover for you.
How do I contact them?
Call 01285 864670 and quote HEALIX.
What do they cover?
Usay Compare will get to know your unique individual requirements, do all the hard work comparing prices and policies for you; then advise on the best and most cost-effective quote.
To find out more about Usay Compare, fill in this online form.
These terms are offered to you as a previous member of the healthcare scheme and are available for a limited time only, usually no more than 30 days from the date of leaving. It is therefore important that you act quickly to maintain continuity of cover.
Health Services Ltd is an introducer appointed representative of both National Friendly and Usay Business Ltd, who are authorised and regulated by the Financial Conduct Authority. Calls may be recorded or monitored for quality control.
How to make a complaint
It is always our intention to provide a first class standard of service: however, we recognise that on occasions, your requirements may not have been met.
Should you have any cause for complaint, you should contact the claims helpline.
How your complaint will be handled
Stage 1
You will receive a written acknowledgement of your complaint within five business days of receipt. This will include the name and job title of the individual handling the complaint.
Stage 2
Within four weeks of receiving your complaint, you will receive either:
-
a final response or
-
a holding response, explaining why we are not yet in a position to resolve the complaint and indicating when we will be making further contact (this will be within eight weeks from receiving the complaint)
Stage 3
If you have not received a final response within four weeks, by the end of eight weeks after receipt of the complaint, you will receive either:
-
a final response.
-
a response explaining why we are still not in a position to provide a final response and explaining when we believe we will be able to do so
-
if we are unable to provide a final response, due to the delay which has now occurred, you may refer your complaint to the Trustees
If, during stage 2 or 3, we issue our final response but you remain dissatisfied, you may refer your complaint to the Trustees. To do this, please set out your reasons fully in writing to the Operations Director, asking for referral to the trustees for further consideration.
How to claim reimbursement
How to claim for cash benefits
If you have received eligible treatment free of charge on the NHS you may be eligible to receive reimbursement of cash benefits as detailed in your table of benefits.
These benefits will only be eligible if the treatment received would otherwise have been eligible for benefit under your scheme.
Please note; only one cash benefit reimbursement can be claimed per admission.
In order to claim these benefits you can register your claim via the Member Zone or the My Healix app.
You will need to provide the following information for a claim to be processed:
- a copy of your NHS discharge paperwork which should confirm the following information:
- date of admission and discharge from the NHS hospital
- name and date of birth of the person admitted to hospital
- summary of the reason for admission and the treatment received
- bank details for the reimbursement to be made to
- account holder’s name
- sort code
- account number
How to claim baby cash benefit
Following the birth or adoption of a child you may be eligible for a cash benefit as detailed in your table of benefits.
In order to claim this benefit you can register your claim via the Member Zone or the My Healix app.
You will need to provide the following information for a claim to be processed:
- a copy of the full birth or adoption certificate
- bank details for the reimbursement to be made to
- account holder’s name
- sort code
- account number
How to claim reimbursement of medical expenses
If you have paid a provider directly for eligible medical services you can claim a reimbursement of these costs as long as the treatment received is eligible for cover as detailed in your table of benefits.
In order to claim this benefit you can register your claim via the Member Zone or the My Healix app.
You will need to provide the following information for a claim to be processed:
- an itemised receipt confirming the following information:
- date treatment was received
- details of the treatment received
- amount paid for the treatment
- bank details for the reimbursement to be made to
- account holder’s name
- sort code
- account number
Please note:
Once the claim has been confirmed as eligible by the claims team, reimbursement will be arranged via direct bank transfer.
All reimbursement claims (including cash benefit claims) must be submitted within six months of your treatment date / birth or adoption date.
Additional information can be found in the payment of invoices page.
Payment of invoices
All treatment should be authorised in advance, so that we can place a guarantee of payment with your healthcare provider, subject to your benefit limits and our reasonable and customary fees. If you have pre-authorised your treatment, we will settle the bill (up to applicable limits) directly with your specialist, therapist or hospital. You are responsible for making sure we have all the information we need to pay your claims.
In some circumstances it may be necessary for you to pay for pre-authorised treatment yourself, and request a reimbursement from us for the cost of the treatment. In these cases please send us a copy of your receipt via email, along with your bank account details, and we will arrange reimbursement via bank transfer. All reimbursement claims (including cash benefit claims) must be submitted within six months of your treatment date / birth or adoption date.
We will not pay for claims:
- if the invoice or reimbursement claim (including cash benefit claims) is not submitted within six months of your treatment date / birth or adoption date
- if the treatment takes place after you have left the scheme
- if you break any terms and conditions of your membership
- if you incur a fee for non-attendance or late cancellations
Requests for additional information
We may ask you to provide information to help us assess your claim. For example we may ask you for one or more of the following:
-
medical reports and other information about the treatment for which you are claiming. If we request a medical report from your specialist and they charge for providing this we will pay the cost
-
original accounts and invoices in connection with your claim
-
obtain results of an independent medical examination or second opinion for which we may ask you to make an appointment with a with a specialist. We will pay for the cost of any independent medical examination or second opinion we require and we will authorise this in writing, in advance
-
provide results of any second opinion you have independently sought under the care of another specialist. On such occasions we may additionally request our own, independent, second opinion from an expert in that field to assess eligibility of cover. We will pay the costs of any second opinion we organise on your behalf, this includes the cost of the consultation and any tests undertaken as a result of that consultation
We will liaise with you and your medical specialists throughout your treatment and will request medical information, when we deem this to be necessary for the assessment of your claim. You will be asked for your consent before we do this.
Throughout your claim we will make you aware of the options that are available to you. If your medical specialist recommends treatment, you should contact the claims helpline as soon as possible to be sure that continued treatment is covered.
Our team of case managers will assess the level of cover available to you for planned treatment within the terms and conditions of the scheme. In some instances it may be necessary to refer your claim to our specialist nurses, along with our panel of independent specialist advisors, who will advise on the level of cover available for the recommended treatment.
Duplicate cover
You must tell us if you are able to make a claim for the cost of any of your treatment from anyone else either under another healthcare scheme or under an insurance policy. For example, if you received an injury that was caused by someone else such as a road traffic accident in which you are not at fault, the scheme will only pay a share of the total costs as appropriate.
If benefits are claimed for treatment to you when the injury or medical condition was caused by a third party, the scheme shall, at its own expense, have the right to pursue such claims in any way considered appropriate in your name. You must co-operate with all reasonable requests in this respect and advise us of any amount you recover directly from the third party.
Healix privacy notice
If you would like to know more about how Healix store and process your personal data, please find our Privacy Notice by clicking here.
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <
Treatment
Treatments
Trust Deed
Trustee, Trustees
United Kingdom
Waiting Period
We, Us, Our
You, Your
Gender Dysphoria
Gender Incongruence
High risk activities
Scheme
Pandemic
Epidemic
Neurodevelopmental disorders
Member Zone
Contacting us
The Healix Team
Our experienced claims team are available to advise and help you, who can be contacted on the helpline number below:
Email: diageo@healix.com
Monday-Friday 08.00-19.00 (Excl. bank holidays)
Saturday 09.00-13.00
Telephone calls to and from our organisation are recorded for the purposes of quality and training.
Any correspondence should be sent to the following address:
Claims Administration Department
Healix Health Services
Healix House, Esher Green
Esher, Surrey
KT10 8AB
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <
Treatment
Treatments
Trust Deed
Trustee, Trustees
United Kingdom
Waiting Period
We, Us, Our
You, Your
Gender Dysphoria
Gender Incongruence
High risk activities
Scheme
Pandemic
Epidemic
Neurodevelopmental disorders
Member Zone
Scheme Year 2026
The below changes will come into effect following the scheme renewal on 1st January 2026.
| New Benefit Name | Benefit Limit | Benefit Wording |
|
Excess |
£100 per member per scheme year |
All members are liable for an excess of £100, payable once per scheme year if you make an eligible claim. The excess will be applied to the first eligible treatment you receive in each scheme year, regardless of when the last excess payment was made. This applies whether the treatment is for the same condition, a related condition, or for an entirely new condition. To ensure clarity, contact us before receiving any treatment (including consultations, diagnostics or therapies) to confirm when the excess will apply. |
|
Further - Precision Cancer Service |
Limited cover |
Please click here for further information. |
Scheme Year 2025
The new scheme year will renew on 1st January 2025. There will be no changes to the scheme for this year.
Scheme Year 2024
The below changes will come into effect for the new scheme year from 1st January 2024.
| Benefit Changes | Previous Wording | New wording |
|
Virtual GP |
Please refer to the Virtual GP page for further information on how to access this benefit. |
This service will no longer be available via Healix but will be provided by Legal and General. For any further information on how to access this service, please refer to the Virtual GP page. |
Section 9: Glossary
The words and phrases below have the following meanings. They will appear in bold in this guide.
Active treatment
Acute condition
Annual renewal date
Benefit
Benefits
Biological therapies
Cancer
Chronic condition
Complementary practitioner
- Acupuncture practitioners must be registered with the BMAS (British Medical Acupuncture Society), BacC (British Acupuncture Council), AACP (Acupuncture Association of Chartered Physiotherapists) or AAC (The Association of Acupuncture Clinicians)
- Osteopaths must be registered with the GOsC (General Osteopathic Council)
- Chiropractors must be registered with the GCC (General Chiropractic Council) <
Daycase
Dependant
-a member’s unmarried dependent children
Dependants
-a member’s unmarried dependent children
Dialysis
- haemodialysis, (through the use of a kidney machine or dialyser)
- peritoneal dialysis (by introducing fluid into the abdomen to act as a filter). <
Disorder
Emergency
Employer
End of life care
General Practitioner
GP
High dependency unit
Home healthcare
Hospital
Private hospital - an independent hospital which can provide acute medical, surgical or psychiatric care. It must be registered under The Registered Homes Act (1984) and approved by the Healthcare Commission or any future law. It may also include a private bed in an NHS hospital.
Inpatient
Intensive care unit
Medical condition
Medically necessary
-
In accordance with professional standards of medical practice in the United Kingdom
-
Clinically appropriate, in terms of type, frequency, extent, site and duration of treatment
-
Required for reasons other than the comfort or convenience of the patient or specialist.
-
Provided at an appropriate facility, in an appropriate setting and at an appropriate level of care for the treatment of the patient’s medical condition.
-
Provided only for an appropriate duration of time.
-
No more costly than an alternative treatment at least as likely to produce the same therapeutic or diagnostic results.
<
Member
Members
Mental health condition
Outpatient
Palliative care
Partner
Physiotherapist
Pre-existing condition
-
you have received medication, advice or treatment, or
-
you have experienced symptoms whether the condition was diagnosed or not.
<
Private ambulance
Prosthesis
Psychological therapist
-
a psychologist who is:
-
Registered with the Health and Care Professions Council (HCPC);
-
Registered with the British Psychological Society (BPS) as a chartered Psychologist
-
a therapist who is:
-
An accredited member of the British Association of Counselling and Psychotherapy (BACP); or
-
An Accredited Member of the British Association for Behavioural and Cognitive Psychotherapies (BABCP); or
-
An Accredited Member of Scotland’s Professional Body for Counselling and Psychotherapy (COSCA); or
-
A practitioner who is registered with the United Kingdom Council for Psychotherapy (UKCP)
Registered nurse
Related condition
Specialist
- a medical practitioner with full current registration with the General Medical Council or
-
a dentist with full current registration with the General Dental Council
and
-
a specialist in the treatment you are referred for (this is applicable to all specialities including anaesthetics and psychiatry)
-
has a certificate of Higher Specialist Training in their specialty that is issued by the Higher Specialist Training Committee of the appropriate Royal College or Faculty
-
is or has been a National Health Service consultant or dentist
-
has been recognised for benefit purposes as a specialist by Healix.
<
Start date
Surgical appliance
The Scheme
Practitioner
- an occupational therapist
- an orthoptist
- a podiatrist
- a speech and language therapist
- a dietician or;
- a nurse who is on the register of the Nursing and Midwifery Council (NMC) and holds a valid NMC personal identification number. <